Two local sisters share an unbreakable bond after bone marrow donation

Lorraine LaRosa faced a seemingly impossible decision.
She knew how fortunate she was to have not one, but three perfect matches for a bone marrow transplant, a procedure used to treat several cancerous and noncancerous diseases, such as leukemia and Hodgkin’s lymphoma. The statistics for finding a perfect match can be grim. The best odds rest in an immediate family member. Otherwise, a patient must rely on the bone marrow registry and the slim chance of matching with a stranger.
Ms. LaRosa had the benefit of a large family. Out of seven siblings, four were healthy enough to be tested. And three came back as matches: her sisters Jennifer Lappe and Melissa Senatore, who live in Calverton, and her brother Jason Klinge of Southampton.
“I was in tears because I didn’t know what to do and who was the better choice,” Ms. LaRosa said.
A sense of urgency had arrived in early 2020. Ms. LaRosa, 62, who lives in Mattituck, was undergoing frequent blood transfusions due to a lack of platelets and low red blood cells.
“Things were getting pretty bad at that point,” she said.
She didn’t want to put the burden on any of her siblings. She called her doctor to talk through her concerns. The time had come to move forward, so the doctor took the decision out of her hands.
After careful evaluation of all three siblings’ health and medical histories — and considering Ms. LaRosa’s worsening situation — the doctor’s choice became clear. The donor would be her sister Jennifer.
Ms. Lappe understood her sister’s hesitancy to ask forsuch a serious commitment. But there was never a moment of doubt. She had seen her sister struggle for years with her illness and have to endure the uncertainty of misdiagnosis and multiple procedures.
“I knew she was scared,” Ms. Lappe said. “I’d be scared with what she had to go through. But she’s a lot stronger than I think she thinks she is.”
Ms. LaRosa texted her sister with the news that “unfortunately” she would be the donor.
“To me there was never a question,” said Ms. Lappe, 60. “I’ll do whatever you need. I’m in a million percent. I said, ‘I’m selfish, I love you. I want you to be around forever.’ ”
The sisters, who were always so close from a young age and grew up in a tight-knit family, would soon form an unbreakable bond — one saving the other’s life.
Before Ms. LaRosa received an ultimate diagnosis of myelodysplastic syndrome, or MDS, in February 2020, she endured years of joint pain and symptoms that seemed to mystify her doctors. One time when her shoulder hurt, she was told it was a torn rotator cuff, which turned out to be inaccurate. Before that, when she was struggling to walk with swollen feet, a podiatrist said she had a torn Achilles tendon, but she hadn’t done anything that seemed to warrant an injury typically seen in athletes. Lupus was also incorrectly diagnosed.
She struggled on a continual journey from one doctor to another.
She ended up in an emergency room on Feb. 27, 2017, and a doctor there noticed that her platelets — the smallest blood cells — seemed low.
Two months later, a doctor at New York Cancer & Blood Specialists diagnosed large granular leukemia, a rare cancer of white blood cells. As time went on, however, her condition did not improve.
Ms. LaRosa’s daughter, Taylor, described her mom as a fighter who was always optimistic and never overly concerned about her health issues.
“I was more so the worrywart,” said Taylor, 29. “I kind of forced her to go to all these appointments and all of these doctors chasing all of these kind of vague symptoms. No one could kind of come up with what was going on.”

A 2009 Mattituck High School graduate, Taylor works as a physician assistant at Weill Cornell Medical Center in New York City. She connected her mom with Dr. Gail Roboz, who specializes in hematology/oncology, in November 2017. Dr. Roboz became well known as the doctor for Robin Roberts, an anchor of ABC’s “Good Morning America,” who was diagnosed with MDS in 2012.
“[Dr. Roboz] kind of took on my case and was monitoring me and was saying my blood didn’t really make any sense,” Ms. LaRosa said. “There were mutations in my blood that weren’t making sense for the large granular leukemia diagnosis.”
Extensive testing revealed that Ms. LaRosa had a predisposition to MDS, a bone barrow disorder and blood cancer that often goes unrecognized and under-diagnosed, according to the MDS Foundation.
“Then it was kind of a weird watching and waiting game,” Taylor said. “I think we all hoped it couldn’t turn into this [MDS], but we knew it could.”
Low-risk patients who do not receive a bone marrow transplant face an average survival rate of up to six years, according to the MDS Foundation. High-risk patients face as little as five months.
Taylor said she braced herself for the possibility that her mother would need a bone marrow transplant at some point. Each December, her mother would undergo a checkup with her oncologist.
Taylor examined her mother’s lab work after the December 2019 appointment and could see the results were abnormal. The family had booked a cruise around Christmastime, so Taylor reached out to her mother’s oncologist to see if it would be safe to travel.
Dr. Roboz gave them the OK and said they’d deal with it when they returned.
“We went on this cruise and I didn’t know anything,” Ms. LaRosa said. “My husband didn’t know anything, but my daughter had all this information. … She had some emotional moments on the cruise. Now, looking back, I know why.”
Taylor recalled the trip to the Bahamas like something out of a movie, where nothing went wrong.
“It was like a perfect trip,” she said.
When Ms. LaRosa returned to her doctor for a follow-up, the reality of the situation set in. Dr. Roboz referred her to Dr. Tsiporah Shore, who has expertise in bone marrow transplants, at Weill Cornell Medicine. They met on March 14, 2020.
“She basically said we need to do this right away,” Ms. LaRosa said. “Things were really progressing.”
Ms. Lappe could see her sister’s health was declining.
“Nothing they did was making her better and I know this was something she dreaded doing,” she said.
Before determining who would be the match, Ms. Lappe said she underwent the most extensive testing of her life. To find a match, doctors analyze the patient’s tissue type, specifically the human leukocyte antigen, or HLA, tissue, the proteins found on most cells in the body, according to the nonprofit organization Be the Match.
Finding the match is just the initial step in assuring that the donor is suitable for the transplant and there are no other potential ailments that could be passed on.
Ms. Lappe had assumed her brother Jason would be the pick since she had an autoimmune disease and he did not. When she found out she had been selected, it coincided with the early stage of the pandemic. That added another layer of stress, since Ms. Lappe knew if she came down with the virus, it could upend the entire process.
Other questions loomed over her.
“You’re worrying, is my body going to do what it needs to do? Is it going to work? Will her body reject it?” she said.
To begin the donation last July, Ms. Lappe received injections to increase her white blood cell count. At the same time, her sister was undergoing radiation and chemotherapy to essentially wipe her immune system clear, eliminating a lifetime of protections that had been built up.
Ms. Lappe said she had been warned she’d feel pain in her bones from the shots. When she didn’t feel anything after the first shot, she worried it might not be working.
By the third and fourth shot, there was no mistaking the odd sensation.
“You have these bone pains,” she said. “I’ve never had that happen.”
On the fifth day, the doctors did a blood test as the final determination to begin the donation process.
Learn more
To read more about bone marrow donation, visit BeTheMatch.org.
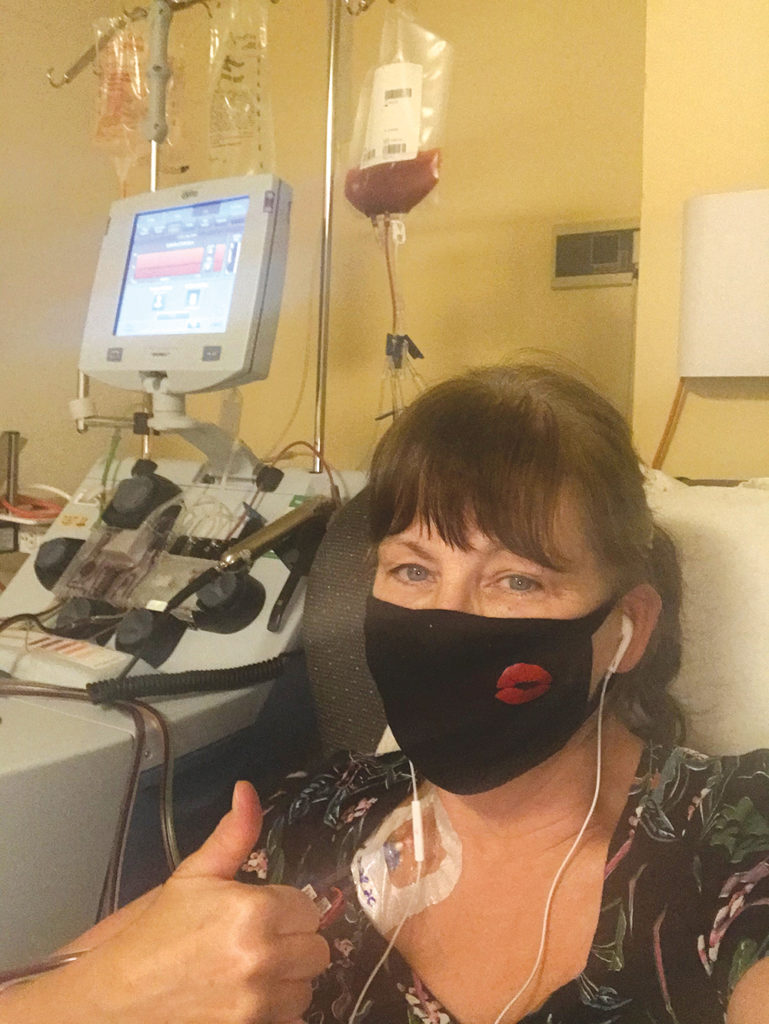
The procedure, called peripheral blood stem cell donation, required Ms. Lappe to be connected to a machine for six hours as blood was removed via a port in her chest to separate out the blood-forming cells. The remaining blood circulated back into her body.
At the end of it, one bag of the pinkish liquid that would be used to save her sister had been accumulated.
“I said to her afterwards, it was so emotional,” Ms. Lappe said, adding that she knew she would feel an overwhelming sense of guilt if the procedure didn’t work.
She took a picture of the bag and its label, which read, “Donor: Jennifer Lappe” and “Recipient: Lorraine LaRosa.” She texted the picture to her sister and said, “Oh, my gosh.”
Ms. Lappe finished her donation on a Wednesday and her sister began to receive her bone marrow the next morning, once the doctors had determined they had a sufficient number of stem cells to start the process.
Then the waiting game began.
The day of a transplant is Day Zero. Every day afterward continues an upward count toward engraftment, when the blood-forming cells received during the transplant begin to grow and create healthy blood cells.
“I would say those days were the hardest, just waiting,” Taylor said. “They would draw her labs every morning at 4 a.m. and the results would be back at 6 a.m.”

A nurse would write the number on a board, and for several days it remained at zero. To pass the time, Ms. LaRosa would play games like Yahtzee with her husband, Mark, who commuted each day into the city. Taylor would watch Netflix shows like “Jane the Virgin” with her mom. The days were largely a blur for Ms. LaRosa.
Taylor knew it could take one to two weeks for engraftment to begin. It was Day 11 when they saw the first sign of hope as a nurse wrote .1 on the board, signaling the first sign of growth.
“I remember that day being like a huge relief and huge turn,” Taylor said.
Ms. LaRosa spent over a month in the hospital for close monitoring as her counts continued to climb. Even after she was released, she had to stay at a nearby hotel for another week because of daily checkups. She set her sights on Day 100, another milestone moment in the recovery.
“If you make past Day 100, it’s a good thing,” she said.
Even after a successful procedure with a 100% match, there’s never a moment of being entirely in the clear. Ms. LaRosa will continue to be monitored for the rest of her life and setbacks are always possible. She’s faced one setback already, with graft vs. host disease, which can be common after a bone marrow transplant. She’s also endured blood clots.
But the biggest thing is that she’s now clear of MDS and feeling better than before the procedure. She still, however, faces residual effects from chemotherapy. She’s often tired.
When she returned home, she mostly stayed inside, unable to venture out with the threat of COVID-19 still hanging over everything. Her immune system was rebuilding from scratch. She remains on a special diet. She can’t have plants in the house, which put her at risk of exposure to pathogens that can cause disease. She can’t have alcohol.
“I said, ‘God, I really want a glass of wine,’ ” Ms. LaRosa said with a laugh.
Taylor said there are constant signs of progress. Her mother just recently had a port removed from her chest wall after close to nine months. She received her COVID-19 vaccine. Her hair is growing back.
“She’s starting to like the style,” Taylor said.
She looks forward to the next steps of returning to normal: going to a movie theater and eating dinner at their favorite restaurant, Grana in Jamesport. When they sit together and toast their wine glasses, Taylor said she knows she’ll cry. They have always shared a close bond, particularly since Taylor was adopted at around 3 months old after her mother endured years of infertility issues.
“She’s been my best friend and my rock for my whole life,” Taylor said.








